How does our body maintain blood pressure?
By Sarah Willis PhD.
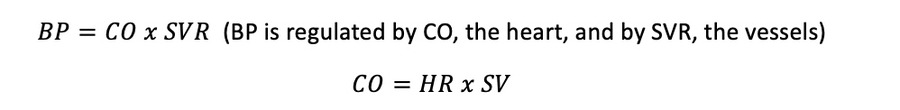
First, we should understand why it is important to maintain blood pressure (BP). A basic need of our body is oxygen, so we need to maintain blood flow to be able to transport oxygen and keep all our systems in function. Then the question would be how do we maintain enough blood flow to adequately deliver oxygen? The answer is related to blood pressure and systemic vascular resistance (in our blood vessels). The body tries to maintain BP and achieve homeostasis no matter what we are doing, for example, exercising/stressed/in pain/etc. It does so through systemic blood flow (CO) and systemic vascular resistance (SVR). See below a couple equations that will help understand this conversation:
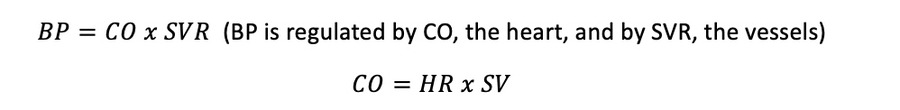
Let’s break that down a bit more. When we are hypotensive (state of lower blood pressure), or in a situation that we need to increase pressure (i.e., due to increased oxygen demand during exercise), our body is responding with the heart and vessels to bring us back to new homeostasis/balance. This is what happens when we increase exercise intensity, the systolic blood pressure goes up. Why? To bring enough oxygen to the muscles and tissues in use. So, how do we do this?
Initially, our baroreceptors (which sense pressure and are in the aortic and carotid sinuses) send a signal to our brainstem  (medulla oblongata and lower pons) to a nucleus of centers. These centers (cardiac acceleratory, vasomotor, and cardiac inhibitory) send signals to communicate with the heart and vessels to regulate/adjust blood pressure to maintain flow and oxygen in system. To increase BP, stimulation of the sympathetic nervous system (SNS) triggers the cardiac acceleratory center to increase heart rate (HR) via increasing sodium to increase action potentials for depolarization, and as well as increasing calcium in the cell to promote contraction and increase contractility – which increases stroke volume (SV). Both HR and SV have influence on cardiac output (CO, systemic blood flow), see equations above CO = HR x SV, and in this case to increase BP (BP = CO x SVR). Furthermore, the SNS stimulates the vasomotor center which allows more calcium into the cell and results in contraction of smooth muscle cells in our vessels. This is called vasoconstriction, which decreases the radius of the vessels and leads to increased resistance. Here we are referring to the equation above with systemic vascular resistance (SVR), which if increased – will increase BP (BP = CO x SVR). A great way to visualize this is with an analogy of a garden hose, as when it is squeezed/kinked, the resistance is increased and the pressure of the water increases. So, when resistance increases, so does BP.
(medulla oblongata and lower pons) to a nucleus of centers. These centers (cardiac acceleratory, vasomotor, and cardiac inhibitory) send signals to communicate with the heart and vessels to regulate/adjust blood pressure to maintain flow and oxygen in system. To increase BP, stimulation of the sympathetic nervous system (SNS) triggers the cardiac acceleratory center to increase heart rate (HR) via increasing sodium to increase action potentials for depolarization, and as well as increasing calcium in the cell to promote contraction and increase contractility – which increases stroke volume (SV). Both HR and SV have influence on cardiac output (CO, systemic blood flow), see equations above CO = HR x SV, and in this case to increase BP (BP = CO x SVR). Furthermore, the SNS stimulates the vasomotor center which allows more calcium into the cell and results in contraction of smooth muscle cells in our vessels. This is called vasoconstriction, which decreases the radius of the vessels and leads to increased resistance. Here we are referring to the equation above with systemic vascular resistance (SVR), which if increased – will increase BP (BP = CO x SVR). A great way to visualize this is with an analogy of a garden hose, as when it is squeezed/kinked, the resistance is increased and the pressure of the water increases. So, when resistance increases, so does BP.

What about when our BP is ‘too high’ in general, or as we recover from a training session or interval? Then the centers in our brainstem stimulate the cardiac inhibitory center to stimulate the parasympathetic nervous system (PNS) and inhibit SNS. This decreases HR by preventing more sodium into the cell (limiting depolarization or contraction) and prohibiting calcium into the cell so there is no/limited contraction to lower SV. Lowering either HR and/or SV will lower CO and consequently BP. Additionally, the vasomotor center is inhibited by the SNS which signals the vessels not to contract – rather relax and vasodilate. Vasodilation increases the radius of the vessel, decreases resistance, and thus decreases BP.
So, it is a huge function of our hearts and vessels to respond to our body’s need to maintain/regulate blood pressure for adequate blood flow and availability of oxygen.
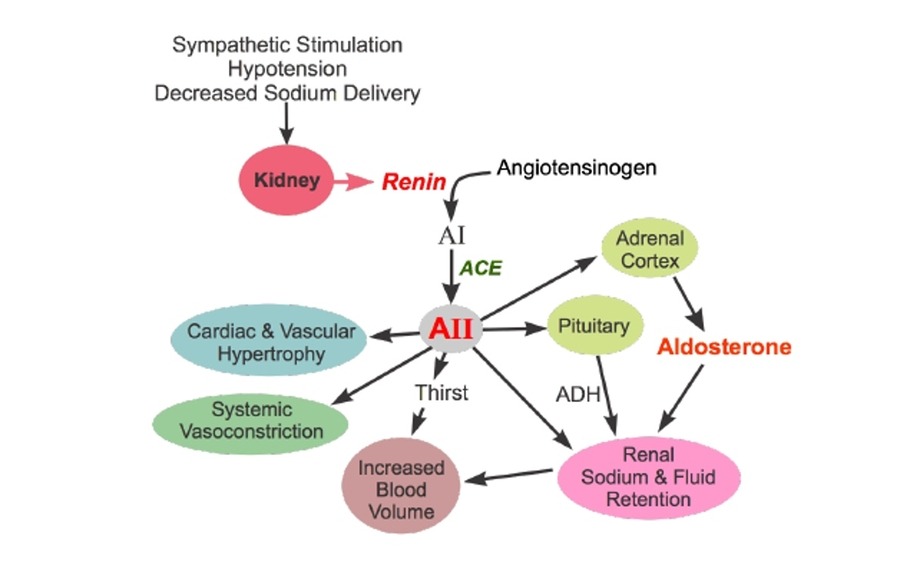
Uniquely, there is another organ that regulates blood pressure, the kidneys. The kidneys have their own detection of blood pressure in the juxtaglomerular cells which stimulate the hormone renin to be secreted. Then renin’s role is to circulate throughout our body, and as it does this it initiates a conversion process from angiotensinogen to angiotensinogen I and then through a converting enzyme to angiotensin II (AT2). AT2 is a powerful enzyme which stimulates many processes which regulate blood pressure, and balance electrolytes and fluids. Specifically, AT2 stimulates secretion of both aldosterone (from kidneys) and anti-diuretic hormone (from pituitary gland in the brain) with the result of retaining or reabsorbing sodium and water to increase blood volume, increase stroke volume, increase cardiac output, and ultimately increase blood pressure. Additionally, AT2 stimulates thirst by which we also arrive in a similar cascade to increased blood volume, stroke volume, cardiac output, and blood pressure. In fact, our blood pressure increases within a few minutes when we drink more fluids, neat! Vasoconstriction of our blood vessels is also stimulated by AT2, therefore, there is decreased radius of the vessel and increased resistance which increases blood pressure.

If we are experiencing hypertension (from exercise, or increased stress/stimulation of the sympathetic nervous system, etc.), then our kidneys also detect this in addition to the left atrium of the heart with secretion of atrial natriuretic peptide (ANP). This hormone, ANP, works to inhibit AT2 and prevent the reabsorption of fluids - so rather, fluids are excreted with increased urination. When increasing urine output, then we decrease blood volume, stroke volume, cardiac output, and therefore decrease blood pressure. Furthermore, when AT2 is blocked, it also stops thirst and doesn’t cause vasoconstriction, so indeed we have decreases in blood volume, stroke volume, cardiac output, and blood pressure. Simply stated, when we drink fluid – our blood pressure increases, and when we go to the bathroom, our blood pressure decreases, fascinating! It is more complex than that, but in a simple way – that is indeed what happens.
Let’s continue to relate this to our ski performance and level of fitness. In a previous article, we discussed that when we work with smaller muscle mass sub-techniques (i.e., double poling versus diagonal stride), our body requires high perfusion pressure and proper vascular conductance. In other words, we demand a rapid delivery of oxygen to the active muscles in combination with impeccable oxygen extraction (ability to off-load oxygen to the tissue cells). So, our body works very hard to regulate blood pressure, especially when using small muscle mass. Let’s expand a bit here…stay with me…when using small muscle mass (particularly with double poling), we have a relatively lower oxygen consumption but have higher blood pressure to keep up with oxygen delivery. Over time, the training of these techniques will improve the oxygen extraction of these muscle groups and translate to increased oxygen delivery which assists with increased tolerance to exercise and efficiency which can improve our maximal oxygen uptake (VO2max). Zoom in a tiny bit more with me to understand that improved oxygen extraction will lower venous oxygen saying that our arterio-venous oxygen difference will increase (VO2 = CO x A-V O2 difference; so increased VO2), yay!
There we go…understanding that training, and thus working on our body’s regulation of blood pressure, improves our efficiency through increasing oxygen extraction and thus improving our oxygen uptake. Time to get back out there and stimulate these adaptations to our cardiovascular system!
