CaRdiovascular Drift
By Tom Cuddy

What is Cardiovascular Drift? And how does it affect training?
My goal for content I contribute to Nordic team solutions is to educate readers on topics related exercise physiology so that the reader can optimize how they train. In the following article, I will be covering some cardiovascular physiology principles so that the reader can more effectively use training tools like heart rate monitors.
A heart rate monitor is a valuable tool for athletes to track exercise intensity across different training sessions. By using preestablished training zones, we can identify the contribution of energy systems being used to fuel exercise (i.e. aerobic vs. anaerobic). This understanding ensures that athletes are training at appropriate intensities considering the intended outcome for a given training session. For instance, during low-intensity, long-distance training, we might have a target heart rate of 65% of our maximal heart rate (HRmax) or below. When implementing this type of training, we are targeting our aerobic energy system, which represents our body's ability to transport oxygen to the highly oxidative type-1 muscle fibers. We train this system to increase mitochondrial density, improve our ability to use fat as a fuel, and to optimize cardiovascular efficiency. Training at a heart rate above this target zone would instead lead to the recruitment of type-2 fibers, and therefore, our anaerobic energy system. This would impair the volume of training we can tolerate during our long days and lead to impaired recovery.
In a perfect world, our heart rate would remain stable throughout a long training day so that pacing would be simple. During prolonged aerobic exercise, cardiovascular variables begin to drift and can cause confusion when using a heart rate monitor. This phenomenon is known as cardiovascular drift.
Before I go into factors that cause cardiovascular drift, let's review some cardiovascular physiology:
During exercise, oxygen consumption (VO2) needs to increase in relation to exercise intensity to fuel aerobic energy metabolism. This increased rate of VO2is a function of increases in cardiac output (Q) and the amount of oxygen the muscles are extracting from the blood. The relationship between these variables is described by the Fick Equation:
VO2= Q x (arterial -venous O2difference)
Cardiac output (Q)is defined by the volume of blood pumped from the heart per minute. This value is determined by stroke volumeand heart rate:
Q = stroke volume x heart rate
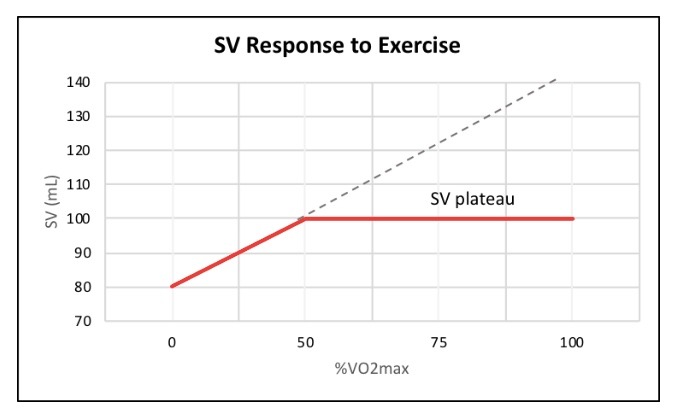
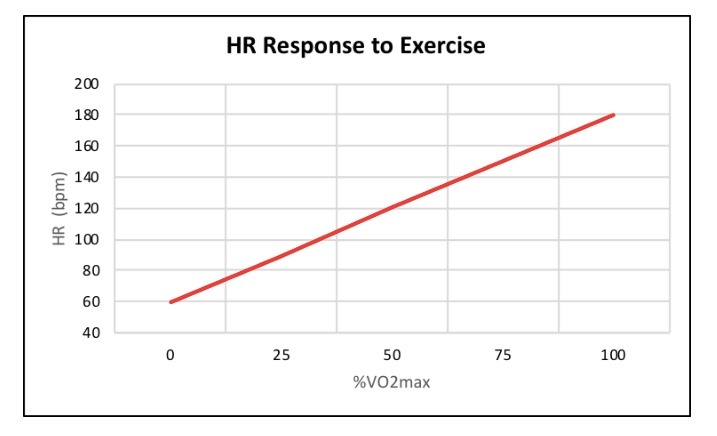
Stroke volume is the amount of blood being pumped throughout the body from the left ventricle per heartbeat. While heart rate is the number of heart beats per minute (bpm). In response to incremental exercise, stroke volume typically increases linearly until it reaches a plateau at an intensity of ~30-50% of VO2max. See below:

Stroke volume plateaus due to the progressive linear increase in HR during incremental exercise. Essentially, when heart rate increases, there is less filling time of the left and right ventricles between each heartbeat. Since the ventricles have less time to fill due to more heart beats, the amount of blood being ejected (stroke volume) decreases. This filling time, known as diastole, is limited when heart rate increases.

To better understand cardiovascular drift, it will be helpful to first identify what physiological factors contribute to an increase in heart rate. These factors are determined by the nervous system, muscle receptors, chemoreceptors, hormones, and thermoreceptors, respectively.
- Upon beginning exercise, there is a withdrawal of parasympathetic nervous system input and a subsequent increased input of the sympathetic nervous system. The parasympathetic nervous system is responsible for inhibiting ventricular contraction to allow relaxation of the heart between heart beats. This "relaxation" promotes longer filling time of the ventricles and less stress on the heart. The sympathetic nervous system stimulates faster rates of ventricular contraction and is upregulated in response to increases in exercise intensity
- When muscle contraction begins during exercise, mechanoreceptors located within the muscle sense changes in muscle length and tension. These receptors then relay this information to the brain to communicate that there is an increased need of oxygen and nutrients. To supply this demand, cardiac output increases as reflected by a higher heart rate.
- When energy metabolism is ramped up at high exercise intensities, metabolic acidosis begins to occur as a by-product of the contribution of anaerobic energy metabolism (see ventilatory threshold article for a further explanation). Chemoreceptors sense this change in the chemical environment and signal the need for increased blood flow to aid in removing the build-up of these waste products.
- To reinforce the sympathetic drive, catecholamines (hormones) - epinephrine and norepinephrine are released from the adrenal gland, which have a cardio-acceleratory effect.
- Another by-product of breaking down glycogen and fats as substrates for muscle contraction is the release of heat. Thermoreceptors throughout the body sense this increase in heat. Our body must quickly dissipate this heat through perspiration (sweating). This increase in body temperature leads to a rapid increase in cardiac output via heart rate in order to send extra blood flow to the skin to regulate body temperature.
Considering what we know about heart rate, why would we see an increase during prolonged exercise at the same pace? In other words, what happens during prolonged exercise that leads to cardiovascular drift?
Let's discuss the example below:
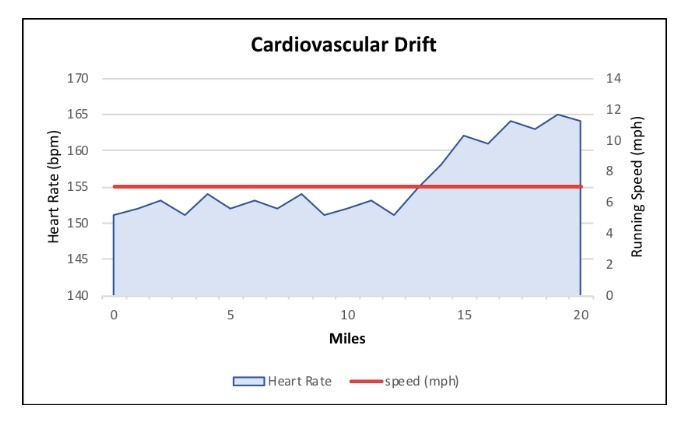
A runner goes out for a 20-mile training run at a speed of 7 mph (8.5 mins/mile). This was considered to be a low-intensity, long-distance run leading up an upcoming marathon. His goal for the training session was to keep his pace at 7 mph and his heart rate below 155 bpm. This heart rate represents the intensity of his 1st ventilatory threshold (VT1), which is the intensity of exercise where anaerobic energy systems begin to be used to fuel exercise. Training below this threshold stimulates adaptation for type 1 muscle fibers and improves fat utilization. If you are unfamiliar with ventilatory thresholds, this heart rate is similar to a zone between zone 2 and zone 3 in a 5-zone model. See polarized training article for further explanation of VT1. For the sake of this example, temperature remained steady at 70 degrees F and it was a completely flat route.

At mile 12, he notices that his heart rate begins to progressively rise. The first part of his run felt incredibly slow so instead of adjusting his pace to keep his heart rate under 155 bpm, he decided to maintain the same pace of 8.5 min/miles. For the last 5 miles of his run, his heart rate stayed between 160 and 165 bpm. At the time of this increase in heart rate, the intensity finally started feeling like a good workout.
Should he have listened to his heart rate and ran slower? Or was maintaining this pace beneficial for his marathon goals? - Let's go into the physiology behind cardiovascular drift to find out.
The cardiovascular drift that occurred on this run is not the result of a faulty heart rate monitor. The primary reason for this spike in heart rate is fluid loss, and therefore, dehydration. Recall that when we exercise, our body temperature rises, and we need to shift blood flow to the skin to release heat by sweating. High sweat rates for prolonged periods of time decreases the fluid content of our blood, known as plasma volume. With a decreased blood volume, there is less blood returning to the heart, and therefore, stroke volume decreases.
As stroke volume decreases, heart rate needs to compensate and increase to maintain the same level of cardiac output.

So aside from him being a little bit dehydrated, this doesn't necessarily answer our question - should he have decreased his pace to keep his heart rate below 155 bpm?
Let's revisit the goal of low-intensity, long distance training days: We train this system to:
- Increase type-1 muscle fiber contraction velocity to improve muscular efficiency. By increasing the "strength" of type 1 muscle fibers, this reduces the need to recruit type 2 muscle fibers at submaximal intensities.
- Increase mitochondrial density for greater rates of oxygen consumption.
- Increase the ability to use fats as a fuel. This adaptation has a glycogen sparing effect, and therefore, leads to a tolerance of greater exercise intensities before needing to tap into "precious" glycogen stores.
During prolonged steady state exercise (>2-3 hours), reusing the same type 1 muscle fibers repeatedly will lead to muscular fatigue. This type of muscle fiber is indeed known as fatigue-resistance, however, after hours of repeated contractions, these muscle fibers can no longer produce adequate amounts of force to sustain exercise demands. The reasons underlying fatigue are multi-faceted and involve cellular, neural, and hormonal changes after hours of exercise.
When active type-1 muscle fibers can no longer produce enough force to sustain metabolic needs, fast-twitch muscle fibers must be recruited as a compensation to maintain adequate force output. The result of increased type-2 muscle fiber recruitment is a greater reliance on anaerobic energy metabolism. Glycogen is used at a faster rate, and therefore, more lactate and metabolic waste products are released. This changes the chemical environment (i.e. a more acidic environment), produces more heat, and puts more strain on muscle. The cardiovascular system must then increase cardiac output to deal with the stress of these changes.
Going back to our example, this change in energy metabolism is reflected by the increase in heart rate towards the end of the training session. By maintaining heart rate instead of pace, this runner would have continued to improve his energy systems related to endurance (i.e. type 1 muscle fiber contraction velocity). Not only should this runner have decreased his pace when noticing cardiovascular drift, but I would argue that his pace in the beginning of the run was simply too close to threshold. This imbalance in intensity would certainly affect this athlete's recovery and possibly lead to impaired training days later in the week. Repeatedly training like this week after week can be a one-way ticket to burnout and possibly overtraining.
Some take-aways:
- A sudden rise in heart rate despite no changes in exercise intensity indicates that hydration needs to improve to avoid dehydration.
- Observing cardiovascular drift demonstrates that there has been a switch in the predominant muscle fibers and energy systems being used (aerobic ®anaerobic).
- If your goal is to train your aerobic energy systems during a low-intensity, long distance training session, there is no long-term benefit to training above threshold.
- More pain doesn't always mean more gain.
