COMPARTMENT SYNDROME (ECS) In SKIING
EXERTIONAL COMPARTMENT SYNDROME (ECS), WHAT IS IT AND CAN WE AVOID IT?

Part 1
By Kurt Jepson
Chronic Exertional Compartment Syndrome (CECS or ECS for short) involving the lower leg, is a diagnosis no athlete wants to hear from their medical practitioner. Its occurrence in Nordic skiing has been on the rise over the last 20 years and despite a surge in research focused on identifying its root cause, ECS remains a bit of a mystery.
Chronic compartment syndrome is not a new pathology. Mavor published a paper describing lower leg ECS in the British Journal of Bone and Joint Surgery in 1956. Numerous works followed after 1973. ECS is not specific to the lower leg. Forearm involvement in production workers is described in occupational medicine literature. In general, there is more research on Acute Compartment Syndrome (ACS) resultant of traumatic input (fractures or crush injuries) to the upper or lower extremities. ACS is very serious as accumulating pressure from intercompartmental bleeding can quickly lead to ischemia and potential limb loss. ECS is rarely a time sensitive issue but should not be ignored either.
This article will look at the epidemiology, pathophysiology, differential assessment and management of ECS involving the lower leg. More importantly in part 2, we`ll look at potential training strategies to possibly limit one`s exposure to this potentially career limiting problem.
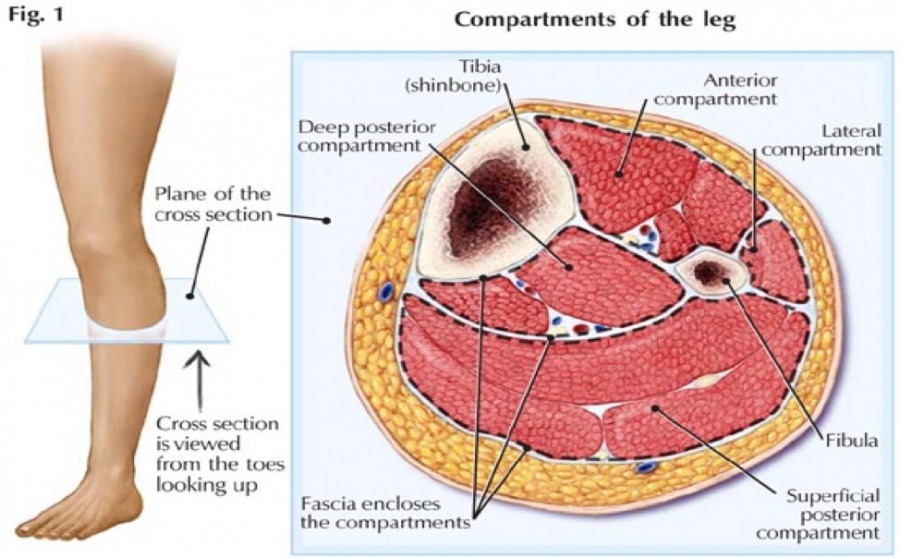
First, basic anatomy. Our “leg” (limb below the knee) is divided into individual compartments bordered by facial tissue and or bone. Fascia is a very unforgiving tissue designed to protect and support delicate underlying soft tissue structures, think “grizzle” in a cut of beef.
Anatomists describe four or five distinct compartments which house nerves, arteries and muscle tendon units. These are basically “closed” environments and as such tissue and circulatory pressures are dictated by available volume and relative expansive capabilities of the “walls” of each compartment.
Normal homeostatic capillary pressures within the compartments typically range between 20-30mm Hg with interstitial tissue pressure below 15 mm Hg.
In 1975 Ashton, et al described the “Critical Closure Theory”, which stated that pressures in excess of 30 mm Hg had little effect on larger diameter circulatory structures, but did compromise smaller vessels abilities to retain unimpeded flow dynamics (micro perfusion).
A cross sectional view of these compartments is pictured below;

The anterior and lateral compartments are most frequently involved in ECS. Most epidemiologic research reports that over 60% of ECS involves the anterior and /or lateral compartments. These regions house the Peroneal nerves as well as the Dorsiflexor (Anterior Tibialis) and evertor (Peroneal) muscles. Both groups are vital to Nordic skiing. We recover our skis in skating and drive our limb forward in classic via secondary actions of these muscles (pull foot toward shin). They are also vital to stabilizing our ankle joint during edging, stance and propulsion. Eighty to 95% of ECS cases are bilateral which is important to note when differentially assessing exercise induced lower leg pain.

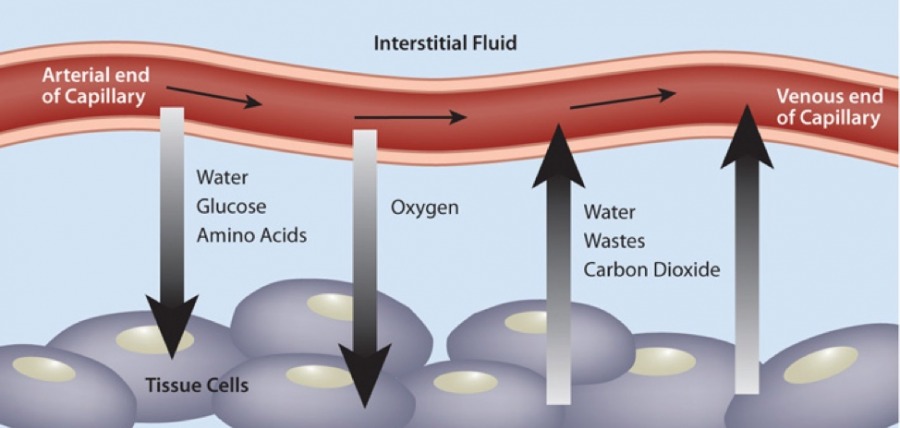
Facial compliance of the compartments is as little as 20% and when muscles expand via work induced perfusion and contraction. Hypertrophy over time further raise pressures within the unit. In 1980 Matsen proposed that an imbalance between the arterial and venous pressure gradient could lead to capillary flow compromise. In short, as pressures rise within the compartment, the thin walled veins are more constricted and compressed than are the thicker walled arteries. Pressures within the venous system rise and compromise gradient capillary bed profusion to working muscles cells. Metabolic waste has difficulty diffusing to a high-pressure venous zone. Oxygen debt (ischemia) and cell death result in inflammation, further adding to compartmental stress and pressures. Chronic dysfunction can lead to scarring. Capillary bed density declines.

This sequence of events was supported in a 2009 morphologic study completed by Edmundsson, et al (Scan J Med Sci Sports, Oct 2009). The investigators took samples of tissue from symptomatic participants during corrective surgery (fasciotomy) and found 30% less capillary density within the associated musculature. At one year follow up, biopsy showed this number had not changed despite a resolution of symptoms and correction of focal neuromuscular damage which was noted at the time of surgery. Fiber type (I II AB etc.) composition between subjects had no effect on the degree of capillary compromise.
These results would seem to shed light on why ECS can reoccur in the post op population, why conservative management usually fails, and presents us with a chicken or egg pathophysiologic question. Does the gradual demise of capillary function via vigorous training/microtrauma lead to ECS or, are individuals with lessor genetically driven capillary bed density prone to developing ECS when the system is stressed?
Epidemiologic data indicates that ECS predominantly affects; athletes under the age of 40, females more than males, those who have undergone a significant alteration in training mode or volume, those with a history of focal leg trauma, and those with any systemic process that compromises circulatory function (i.e. diabetes, vasoconstrictor use, myofascial dysfunctions). It may be more prevalent than suspected. A NYU study (n=150) found that 33% of patients presenting with exercise induced lower leg symptoms were later found to have catheter confirmed ECS. Stress fractures, neuropathies, muscle strains and medial tibial stress syndrome (a form of shin splints) comprised the remaining diagnoses` of the group.
Physical examination of ECS patients is difficult and assessment is typically arrived at via the exclusion of other pathology. One`s specific history entailing what causes and alleviates symptoms is paramount to the clinical process, and the clinician must take the time to “let the patient tell you what is wrong”. Classic “red flag” symptoms are rapid onset of symptoms with the offending exercise (10-20 min) and rapid resolution of symptoms when at rest (5-10 min). Few musculoskeletal irritations resolve that quickly with sitting and tend to linger post session. Not all forms of exercise are equally provocative. Some people ski with difficulty but run without issue and vice versa. Most cycle comfortably. Recall that 80-95% of ECS is bilateral. Not so for most lumbar, “shin splint” or bony issues.
Specific diagnosis can only be made via intramuscular compartment pressure readings post exercise which specifically induces symptoms (ie roller skiing vs running). Readings must therefore be taken immediately field side or following the provocative activity in a clinical setting. A Wick or Slit Catheter device is inserted and the involved compartmental pressure is measured in mm Hg. Until certain criteria is met, it is not ECS.
Pedowitz, et al (1990) published the pathognomonic scale (below) for determining what pressure readings confirm the suspicion of ECS. This scale continues to guide sports medicine practitioners when devising treatment plans for their patients.
Confirmation of ECS if;
-Resting baseline pressures of 15-30+ mm Hg
-1 min post exercise pressure > 30mm Hg
-5 min post exercise pressure > 20 mm Hg
-Mid exercise pressures > 45mm Hg
MRI studies continue to be conducted to establish/standardize diagnostic criteria, but of course diagnosis via this medium is expensive.
In part two we`ll look at treatment strategies and offer advice on how to minimize any potential for this problem as you plan your summer and fall training sessions.
