Recovery Techniques - What You need to know - Part two
By Kurt Jepson

 There is some concern for the adverse response of Rhabdomyolysis arising from areas that are focally treated for an extended time frame (i.e. > 10 min).
There is some concern for the adverse response of Rhabdomyolysis arising from areas that are focally treated for an extended time frame (i.e. > 10 min).


 Cheng A, Willis S, et al. authored; Post-exercise recovery of contractile function and endurance in humans and mice is accelerated by heating and slowed by cooling skeletal muscle in the J Phys 2017, and looked at the effects of heating (38 deg C), cooling (15 deg C) or not treated (33 deg C) during a 2 -hour recovery period post exhaustive arm cycling.
Cheng A, Willis S, et al. authored; Post-exercise recovery of contractile function and endurance in humans and mice is accelerated by heating and slowed by cooling skeletal muscle in the J Phys 2017, and looked at the effects of heating (38 deg C), cooling (15 deg C) or not treated (33 deg C) during a 2 -hour recovery period post exhaustive arm cycling.
 There is a considerable amount of literature relating the use of sauna bathing and an apparent elevation of growth hormone (GH) and suppression of serum Cortisol (stress hormone). One dated study (Lammintausta et al in the Ann Clin Res, 1976) measured serum GH at 142% over subjects’ baseline while in the sauna. While that number seems suspect, other investigators over the years have identified favorable endocrine responses to sauna use, albeit less pronounced. Commonly identified as “beneficial” hormone variations via sauna use include; the afore mentioned elevated GH, Noradrenaline (the “feed, breed, relaxing” hormone), beta-endorphins (feel good chemicals), Cortisol suppression and renin-angiotensin (blood pressure moderators) to name a few (Kukkonen et al, Podstawski et al, etc).
There is a considerable amount of literature relating the use of sauna bathing and an apparent elevation of growth hormone (GH) and suppression of serum Cortisol (stress hormone). One dated study (Lammintausta et al in the Ann Clin Res, 1976) measured serum GH at 142% over subjects’ baseline while in the sauna. While that number seems suspect, other investigators over the years have identified favorable endocrine responses to sauna use, albeit less pronounced. Commonly identified as “beneficial” hormone variations via sauna use include; the afore mentioned elevated GH, Noradrenaline (the “feed, breed, relaxing” hormone), beta-endorphins (feel good chemicals), Cortisol suppression and renin-angiotensin (blood pressure moderators) to name a few (Kukkonen et al, Podstawski et al, etc).
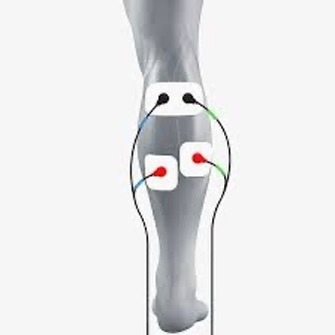 Electrical stimulation has been shown to cause vasodilation along the course of blood vessels (blood flow enhancement), activation of cutaneous sympathetic nerve endings (pain modulation), regional motor unit recruitment not typically activated voluntarily (strength gains), and also limits the regression of capillary tissue post “trauma” (Drummond, Brit J Clin Phar 2007, Figueroa et al Circulation Research 2003, Dobsak et al Circ J 2006, Vanderthommen et al Arch Phys Med Rehab 2002, Tanaka et al J Appl Phys 2021).
Electrical stimulation has been shown to cause vasodilation along the course of blood vessels (blood flow enhancement), activation of cutaneous sympathetic nerve endings (pain modulation), regional motor unit recruitment not typically activated voluntarily (strength gains), and also limits the regression of capillary tissue post “trauma” (Drummond, Brit J Clin Phar 2007, Figueroa et al Circulation Research 2003, Dobsak et al Circ J 2006, Vanderthommen et al Arch Phys Med Rehab 2002, Tanaka et al J Appl Phys 2021).

 There have also been studies investigating the effects of IPC on muscle glycogen (uptake) recovery.
There have also been studies investigating the effects of IPC on muscle glycogen (uptake) recovery.


See part one for introduction. In part two Kurt continues to research common recovery strategies.
MECHANIZED PERCUSSIVE RECOVERY TOOLS
This topic falls into the massage category. Percussive Therapy (PT) via a vibratory device was originated by Robert Fulford in the 1950`s as an osteopathic treatment for musculoskeletal pain. Commercially available devices were availably by 2008. Percussive device treatment mimics “tapotement” massage.

There are many companies who have entered the sports recovery realm and promote their products.
This from an ad placed in a well-known runner’s magazine:
“This massage gun helps relieve muscle soreness with an astounding 15 interchangeable heads, it promotes circulation and improves range of motion, and its brushless motor is super quiet. The massage gun delivers up to 3,200 percussions per minute, making it ultra-powerful, ……”
Given what we know, per the literature, about human delivered soft tissue manipulation, manufacturer claims of “Percussive Massage” benefits should be scrutinized.
Looking at the research, hand held “massage guns” are on par with traditional massage therapy in terms of effecting recovery parameters such as; ROM, performance, regional circulation, DOMS, and pain modulation.

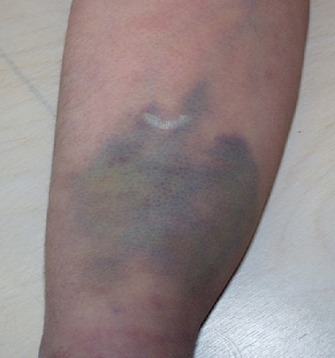
A case report by Chen et al documented the symptoms of a young woman who presented for evaluation complaining of fatigue, thigh muscle pain, and dark urine following coach performed, lower quadrant muscle treatments utilizing a percussive device, for a post cycling session recovery.
Labs identified extremely high creatine kinase levels, an indicator of significant muscle trauma, and urinary hemoglobinuria. Her exam findings included multiple thigh hematomas and exquisite tenderness. She was hospitalized and began an aggressive course of intravenous resuscitation (Rhabdomyolysis after the use of percussion massage gun: A case report. Phys Ther. 2021 Jan 4; 101 (1)).
Investigators from Portugal (Ricardo et al ) published; The Effects of Massage Guns on Performance and Recovery: A Systematic Review, this September in Funct. Morphol. Kinesiol (2023, 8(3)). This study examined the effects of the pre- and post-activity use of percussive guns in a young athletic population. Only 11 out of 281 literature records met inclusion criteria, due to the high rate of bias in many studies. The results were somewhat predictable based on what we know about manual therapy.
Regarding strength, balance, acceleration, agility and explosiveness, the use of “guns” had no effect on performance or in some instances, results indicated performance suppression.
When looking at recovery related outcomes, the use of massage guns was shown to be a cost-effective intervention (verses routine massage therapy) for stiffness reduction and ROM improvements “immediately” after fatiguing exercise protocols. No differences were noted in participant perceived exertion, lactate concentrations, or muscle contraction parameters.
Percussive guns have also been promoted as a warm up tool prior to athletic activity. Theoretically, their use pre-activates or “excites” neuromuscular pathways and raises muscle temperature via imparted mechanical energy and a vascular response. Manual “tapping” techniques have been employed by physical therapists in neurologic settings for decades to enhance muscle activity in hypotonic patients. Anecdotally, spindle reflexes are typically the target of such interventions.

Kujala RP et al looked at these “gun” activating claims in 2019 (The effect of handheld percussion treatment on vertical jump height. Int J of Exer Sci: Con Proceedings. Vol 8 (7)).
Twelve adult trained males comprised the group (n=12). The study group received 5 minutes of stimulation to lower quadrant “jump” groups (calves, gluts, hamstrings, quads) from a therapeutic gun constituted the percussive warm up, after 15 minutes of traditional dynamic activities. Controls performed the 15 min dynamic warm up only. A vertical jump test was performed on all participants. No affect on vertical jump ability was noted. The authors acknowledged the need for larger participant samples.

Conversely, Sams L. et al recently investigated the physiological effects of Percussive Therapy (PT) “guns” via a literature review in 2023. They hoped to determine the effect of PT on such physiologic adaptions as; strength, explosive muscle action, flexibility, and musculoskeletal pain (The effect of percussive therapy on musculoskeletal performance and experiences of pain: A systematic literature review. IJSPT.2023; 18(2): 309-327). Data sources dated from 2006 on, were included if they included language involving adult populations receiving PT. Study inclusion was determined via the Critical Appraisal Skills Programme and PEDro scores.
The authors acknowledged using a board criterion for inclusion, including; primary studies, conference presentations, and Doctoral theses, which could be viewed as a “strength” due to the volume of work, or “weakness” due to a lack of strict peer review for inclusion. They concluded that this PT review did indeed “infer” that PT guns could promote an acute response in strength, flexibility and pain suppression when compared to placebo or no treatment.
The phrase “do no harm” likely holds true for percussive guns, as it does for other manual soft tissue techniques. They can be costly, often running hundreds of dollars. Exercise based pre-event activation, utilizing proven neuromuscular recruitment (i.e. plyo or band) protocols, may be a better option for those with financial constraints. This approach has been discussed numerous times on this site and instructional videos provided within.
COOLING
Local or regional cooling has long been thought a means of assisting muscle recovery. Various “myths” surrounding post exercise techniques such as ice bath immersion have persisted over the years. Cryo-immersion (classically defined as temperatures <15 deg C) has been thought to cause a vasomotor response capable of “squeezing” toxins out of muscle tissue, reduce inflammation and lower cellular metabolic demands.
 Various investigators in the early 2000`s rebutted such claims and suggested that the physiologic effects of regional cooling were limited to, at best, short term performance enhancement if the athlete was stressed in a thermoregulatory, or heart rate sense. There has been suggestion that immersion may trigger a faster return to a parasympathetic, relaxed homeostatic state (Int J Sport Physio Perform 06,08. Int J Sport Med 07. J Sport Sci 08. Am J Physio Heart Circul 09).
Various investigators in the early 2000`s rebutted such claims and suggested that the physiologic effects of regional cooling were limited to, at best, short term performance enhancement if the athlete was stressed in a thermoregulatory, or heart rate sense. There has been suggestion that immersion may trigger a faster return to a parasympathetic, relaxed homeostatic state (Int J Sport Physio Perform 06,08. Int J Sport Med 07. J Sport Sci 08. Am J Physio Heart Circul 09).

Bleakley C et al published an Intervention Review in 2012 which investigated cold-water emersion effects on muscle soreness and fatigue after exercise. They scrutinized 17 clinical trials (n=366) and noted that overall, most studies were of “low” quality due to a lack of standardization of; temperatures utilized , duration, frequency, exercise stimulus, inconsistent post treatment surveillance and environmental settings.
Fourteen of the studies compared immersion to passive interventions and did note that when results were pooled, there appeared to be a small but statistically significant benefit to immersion verses no intervention at 24-, 48-, 72- and 96-hour post exercise intervals. Results favored running induced “soreness” verses other exercise inputs.
Five studies compared cold -water immersion to contrast hot-cold immersion, with no intervention as a control. Investigators identified no variation in pain response of the subjects at 24, 48, 72-hour follow-ups despite the intervention, or lack thereof, used.
Overall, there seems to be some limited evidence to suggest that cold-water immersion verses no intervention, can be justified for the control of pain or muscle soreness related to exercise.
Bleakley concluded that the optimal parameters for immersion techniques have not been identified in the literature (Cold-water immersion (cryotherapy) for preventing and treating muscle soreness after exercise. Cochrane Database of Systematic Reviews 2012, Issue 2).
The difficulties with the “dose” of Cold-Water Immersion (CWI) should be a concern for athletes utilizing this technique to recovery.
Roberts L et al found that use of CWI verses active recovery (ACT) over a 12-week training block, actually impaired study participants isokinetic strength gain, muscle hypertrophy, neural cell activity and kinases activity, all of which translated to suppression of long-term training gains (Post-exercise cold-water immersion attenuates acute anabolic signaling and long term adaptions in muscle to strength training. J Physio. 2015; 593(18)).
A 2016 study by Peake J et al, comparing 10-minute unilateral limb CWI to ACT and the lower extremity muscle cellular inflammatory response to vigorous exercise.
Study subjects (n=9, 18 lower limbs) were their own controls. No benefit to CWI over ACT at the 2-, 24-, and 48-hour marks post exercise was noted. Exercise led to the infiltration of inflammatory cells, neurotrophins, cytokines, and the subcellular translocation of proteins in both groups at equal levels (The effects of cold-water immersion and active recovery on inflammation and cell stress responses in human skeletal muscle after exercise J Physio, 595(3)).
Many athletes combine post exercise nutrition with recovery techniques such as CWI to better manage  time constraints. A 2019 study looked at the consumption of a carb-protein beverage and protein synthesis immediately after subjects (n=12) submerged their post resistance exercised limb in a CWI bath at 8 deg C or, a thermoneutral bath at 30 deg C. Blood and muscle sampling in of limbs over a 5-hour recovery period showed significant inhibition of protein synthesis rates in the CWI limbs compared to the temperate bath limbs. Alarmingly, this trend continued for up to 2 weeks post exercise (Fuchs C et al. Postexercise cooling impairs muscle protein synthesis rates in recreational athletes. J Phys 598(4))!
time constraints. A 2019 study looked at the consumption of a carb-protein beverage and protein synthesis immediately after subjects (n=12) submerged their post resistance exercised limb in a CWI bath at 8 deg C or, a thermoneutral bath at 30 deg C. Blood and muscle sampling in of limbs over a 5-hour recovery period showed significant inhibition of protein synthesis rates in the CWI limbs compared to the temperate bath limbs. Alarmingly, this trend continued for up to 2 weeks post exercise (Fuchs C et al. Postexercise cooling impairs muscle protein synthesis rates in recreational athletes. J Phys 598(4))!

There seems to be considerable data out there which contradicts the use of cold-water immersion as a recovery strategy following vigorous exercise. It appears to be a case of “risk vs reward”. Athletes who routinely use CWI post training should perhaps reconsider this habit.
CONTRAST AND THERMAL TREATMENT
Happily, there is substantial evidence that modalities such as sauna, warm jet tubs, and contrast baths (typically a 3 warm to 1 cold ratio) are efficacious pathways to enhance recovery from DOMS, adverse biochemical parameters, and perceived fatigue (Viitasaio 2007, Versey 2010, J Strength Conditioning Research).

Measures included the fatigability and power output of those muscles involved following recovery. The heated group generated better power with testing than did the cooled group, in fact the cooled group were adversely affected regarding this parameter. Glycogen resynthesis was also enhanced by heating.
The skiers takeaway,….wear your parka and stay out of snowbanks!

ELECTRICAL STIMULATION
Modalities such as electrical stimulation therapy may not be readily available, or affordable to most amateur athletes. Still, this recovery/rehabilitation technique is worth mentioning, especially for those experiencing a regionalized musculoskeletal training related malady such as lumbago.

Electrical stimulation when applied by qualified clinicians (with an electrophysiology background), using the correct physiologic parameters and protocols is an efficacious tool for recovery from local/ regional injury or overuse.
INTERMITTANT PNEUMATIC COMPRESSION
The home and clinical market for “intermittent pneumatic compressive” devices (IPC) has exploded over the last decade. Equipment costs range from hundreds to thousands of dollars per unit. Some combine cryo-cooling aspects as well.
They have been typically employed in medical settings for patients who are experiencing circulatory decline due to systemic illness such as diabetes, peripheral vascular disease (PVD), lymphatic dysfunction, or are post op and at risk for vascular compromise such as deep vein thrombosis (DVT). They have been shown to be effective in these patients, providing favorable outcomes where existing circulatory status is compromised, or, pain modulation is the goal without the extended use of prescription medications (Waterman et at, J Knee Surg. 2012, ACL reconstruction patients. Marinova et al, Knee Surg Sports Trau Arthrosc. 2023, and Block J, Open Access J Sports Med, 2010, total knee replacement patients. Amer Ortho Foot Ankle Society, post ankle foot trauma patients).
The literature is less definitive however regarding their value as a recovery tool in a healthy athletic population, where circulatory function is not an issue. A healthy, athletic circulatory system has an amazing ability to maintain homeostatic vessel pressures, allowing for efficient transfer of metabolites across pressure gradients.
There is often a blurred delineation between “marketing science” and “science- science”, when it comes to IPC. Athletes, coaches, and fitness consultants should be able to critically analyze available peer reviewed research to assist with recovery modality decisions.

The prevailing body of research has revolved around ultra- athletes, triathletes, runners, and cyclists. Studies typically investigate the effects of ICD on the resolution of; short term discomfort, delayed muscle soreness DOMS, exercise induced muscle damage (EIMD), and biochemical markers of physiologic stress.
Stedge and Armstrong published an oft cited review in the J Sports Rehabilitation (2021, 8;30(4)).
In; “The Effects of Intermittent Pneumatic Compression on the Reduction of Exercise-Induced Muscle Damage in endurance Athletes: A Critically Appraised Topic,” they presented their review findings of high-quality randomized studies which looked at IPC `s ability to influence DMOS, acute soreness and plasma creatine kinase (a marker of muscle damage). They concluded that IPC had a limited beneficial effect on short term post exercise discomfort and no influence on creatine kinase levels, processing, or DOMS in populations of marathoners, triathletes, and cyclists.
Draper S. et al, found similar results in terms of creatine reactive protein concentrations and DOMS in runners (n=10). Participants (5 males, 5 females) performed two 20 mile runs at 70% VO2 max. No difference was seen in the IPC groups receiving treatment immediately and for 5 consecutive days post exercise, verses a control/non treated group which received “passive rest” as the recovery strategy (Effects of Intermittent Pneumatic Compression on Delayed Onset Muscle Soreness in Long Distance Runners. Int J Sci. 2020; 13(2)).
O`Donnell and Driller ( J Sci Cycling, 2015; 4(3)) evaluated the effects of IPC use between vigorous training bouts in a population of well-trained triathletes (n=10). They identified no significant differences between an IPC group and a passive recovery group, following completion of two 40 minute “high intensity” cycling trials, with 30 minutes of recovery. They measured blood lactate concentrations, and performance of a 5-k treadmill TT following the second cycling trial.
In a larger sample size study, Wiecha S. et al, took 45 healthy males and had then perform 100 drop jumps to induce adverse muscle load. They were randomly placed in a “sham microcurrent stimulation” recovery group, or an IPC group for 30 minutes of “recovery” following the exercise input.
Measures of; creatine kinase, lactate dehydrogenase, isokinetic strength, soreness, and knee joint motion were evaluated post recovery. No differences in biochemical or functional measures were noted (The efficacy of intermittent pneumatic compression and negative pressure therapy on muscle function, soreness, and serum indices of muscle damage: a randomized controlled trial. BMC Sports Sci Med Rehabil 2021; 13).

In the J Strength and Conditioning Research 2015;29(2), Keck N et al took 10 active males and had them complete a 90 minute “glycogen depleting” ride (cycling). This was followed by 4 hours of recovery with either IPC or passive rest administered at 0-60- and 120-180-minutes post exercise. A carbohydrate beverage was provided at 0 and 2 hours post ride. Muscle biopsies and blood samples were collected at 0 and 4 hours into recovery. There was no difference in muscle glycogen resynthesis during or post recovery, between the IPC or passive recovery groups. Blood glycose, insulin, and lactate concentrations all changed with respect to time post exercise, but did not vary between groups.
There are also IPC verses manual therapy (MT) comparison studies, and their relative efficacy.
Hoffman et al, (JOSPT. 2016) concluded that a single 20-minute session of either IPC or post-race (ultramarathoners) massage provided some subjective relief “immediately” after the physical effort, but there was no evidence that either strategy provided any long term functional or subjective benefit. A 2018 study by Heapy A. et al, had similar conclusions (A randomized controlled trial of manual therapy and pneumatic compression for the recovery from prolonged running-an extended study. Res Sports Med. 2018; 26(3)).
Fifty-six ultramarathoners (n=56) were asked to run 400m prior to their race event and then again at 3,5-,7-, and 14-days post-race/marathon. Post marathon manual therapy (MT) and IPC groups were established and scores for fatigue, soreness, and plasma creatine kinase were documented. Both groups subjectively noted that muscle fatigue was slightly improved with either intervention immediately after the race and on post-race day 1, however, soreness and 400m times were not improved in either group beyond day 1.
Lastly, there appears to be some evidence that IPC used in conjunction with exercise, concurrently, improved Doppler measured superficial arterial blood flow in the calf muscle of 12 subjects (Zuj K et al .J Appli Physiol 2018).
Another study by Haun C et al found that 18 recreationally trained males who performed 3 consecutive days (days 1-3) of high intensity interval training (HIIT) and received 3 consecutive days of IPC (days 5-7) had reduced skeletal muscle markers of proteolysis (break down), but no variation regarding flexibility, 6-k run test results, pain threshold, or serum creatine kinase levels.
These studies might lend support to the practice of intra- /post-sport compressive garment use. Perhaps a topic for future investigation.
ACTIVE RECOVERY
So, given all that we know about recovery strategies, what provides the athlete with the most ‘bang for the buck”, especially if time, access, and financial constraints mandate choosing THE most effective recovery technique? I suspect you already know ,and hopefully commit to it after any hard training or race effort.

Jogging, cycling, water exercise (Cortis et al Int J Sports Med 2010), easy calisthenics, “flow” yoga, an easy ski, etc. all provide stimulus the body requires to return to a homeostatic state, setting the stage for super-compensation. The activities selected should of course involve those muscles just utilized for the training effort and should be combined with early nutrition.
Early work by Coso, Baldari, Riberio and others established that “easy” work with an intensity ~30% VO2 max and a ventilatory threshold of ~10% worked best for reversing hyperlactemia and for CO2 offloading post exercise. More than 20 minutes of easy activity proved to have no advantage, and in fact there was a point of diminishing return if the duration was extended out to ~1 hour.
Those early parameters seem to be holding up to scientific scrutiny. Active recovery is more beneficial to negating long term soreness (lasting days not hours), performance, subjective wellness, and blood lactate (La) clearance, when compared to passive rest or massage, etc. in numerous works. Most studies support a recovery work intensity of between 30-40% VO2 max for efficient La clearance (Dodd et al J Appli Physio 1984, Stamford et al J Appli Physio 1981, Gupta et al Int J Sports Med 1996, Weltman et al J Sports Sci 2013, Mika et al PLOS one 2016). Twenty to 40 minutes duration seems to provide optimal results, with longer recovery efforts providing no additional benefit, aside from one study by Menzies et al ,(J Sport Sci 2010) finding La clearance occurred more rapidly at 60-100% of lactate threshold.
The obvious advantage to active exercise as a recovery tool is it’s; simplicity, availability, affordability, and efficacy. Think of it as the Chocolate milk of musculoskeletal and biochemical recovery (Lunn W et al. Chocolate Milk and Endurance Exercise Recovery: Protein Balance, Glycogen, and Performance. Med Sci Sport and Exer. Aug 2011)!

Recovery is without argument, an essential part of performance enhancement. As with so many other topics related to sports physiology, there is rarely a specific “cookbook” for every athlete to utilize.
The informed athlete will mix a measured dose of anecdotal “it works for me” along with scientifically tested techniques, resulting in a recovery process that allows for super-compensation and physiologic progression.
If time and money are precious commodities for you, utilize science over anecdote.
Go find some racin`!
Kj
