Compartment Syndrome (ECS) in cross country skiing

April 21, 2019
By Kurt Jepson
In Part 1 we looked at the anatomic and physiologic features that pre-dispose one to ECS given sufficient provocative training input. Diagnosis is best confirmed via a pressure sensitive catheter inserted into the involved compartment prior to, post, or ideally midsession as the athlete reproduces their symptoms. As mentioned previously, symptoms can vary from individual to individual as can the specific pathomechanical activity.
Most athletes describe a sense of weakness or “floppiness” of their ankle and foot as the offending activity progresses. Foot drop or “slap” at heel strike while running or the inability to clear the shovel of the ski from the snow while skating are common complaints. Pain varies from negligible to intense and typically centers on the anterior (front) and/or lateral (outside) of the lower leg. Any of the 4 compartments described in Part 1 can be involved. Most cases involve the anterior (Dorsiflexors) and lateral (Everters) compartments. Pain can be widespread across the entire compartment(s) with accompanying “spasm” or simply isolated symptoms just above the ankle complex. Many describe “tightness” in this region, “like a band wrapped around my leg”. Transient (tingling) are common in advanced cases.
The time to symptom onset varies from a few to many minutes of exercise participation. Typically, less time is required to cause irritation the more advanced the issue. A keynote factor involved in the differential assessment of ECS is the time required to resolve symptoms once the offending exercise ceases. Symptoms clear rapidly in ECS once the athlete rests (usually within 15 mi +/-). Few musculoskeletal issues resolve rapidly with rest, tend to linger for hours once provoked, and resting pain into the next day is common based on severity or chronicity. Recall that ECS tends to be bilateral, most musculoskeletal issues are unilateral.
The exact source of one`s pain is unclear. Many investigators have hypothesized that inadequate perfusion leads to aberrant neurosensory activity, but the experimental pressures required to significantly impeded microcirculation in studies vary from ECS diagnostic thresholds to 200mmHg (Styf, Amendola, Balduini, Trease). Some suspect noxious facial load from forced expansion as the origin of pain.
It is important to get an exam by a sports medicine practitioner if symptoms are chronic, interrupt normal daily activity, disturb sleep, include nocturnal cramping, or are recalcitrant in spite of treatment attempts. There are serious lower leg pathologies which should be excluded in a timely fashion such as; lumbar based radiculitis, proximal vascular entrapment, infection, neoplasms, and pathologic fractures to name a few. Children with ongoing symptoms should most certainly be examined.
Physical exam, as mentioned in Part 1, is primarily exclusionary in focus. Fractures and “shin splints” have very different responses to exam tests than does ECS. In some cases, unusual hypertrophy of the anterior compartment may be noted with or without localized “bulges” due to fascial herniations. Tactile sensation is usually intact. Ankle /foot pulses may be suppressed in severe cases. Tenderness is usually present. Associated compartmental muscular weakness can be quite pronounced. Surface EMG is typically unreliable.
Conservative management attempts over the years for confirmed ECS have produced poor outcomes. Rehabilitative exercise and soft tissue work have been shown to delay the onset of symptoms in patients but have no effect on compartmental pressures or problem resolution (Blackman 1998). Surgical intervention (fasciectomy or fasciotomy) produces the best long term result but does require a lengthy post op convalescence. Satisfaction rates for anteriolateral release surgeries have been reported to be as high as 96% (Schepsis et al 2005). Posterior release results are less favorable.
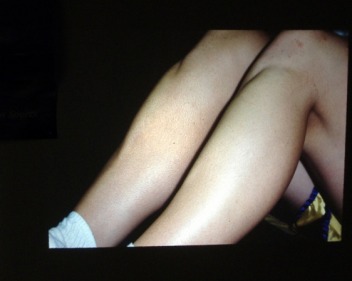
(note the pronounced muscle bulk anteriorly in this symptomatic HS female soccer player)
So, what are some strategies Nordic athletes and coaches can employ to limit the chances of having to deal with ECS?
This time of year is particularly pertinent to this topic, as athlete training plans are designed for spring and summer use. Too much too soon goes without saying, as does the relative percentage of L1 verses L3-5 exposure. There is no firm data related to whether extensive cyclic loading (L1) or vigorous loading (L5) is more contributory to ECS. Cases are reported in marathon runners and soccer players. That said, the mix and dosage of specific training modes must be carefully thought out.
Youth training plans should adhere to the USSA XC age/phase specific Training System available online via the education resources section at USSA.org.
Over distance (OD) workouts should be primarily completed via road cycling. A 1993 study by Beckham et al found significantly higher baseline compartment pressures in runners compared to cyclists, although there were no “significant” differences in pressure elevation following sustained exercise at 80% of VO2 max. They did find however find that creatine phosphokinase markers anterolaterally were ten times elevated in the running group compared to the cyclists. Food for thought if one wishes to avoid muscular microtrauma and possible physiologic sequelae on a repetitive basis. Trail running, hikes and mountain biking certainly have value and can logically be included in one`s overall training plan provided they don`t dominant one`s OD sessions.
Roller skiing should be equally divided between classic and skate techniques with perhaps a bias toward double poling (DP). Equipment should be in good repair to avoid excess loads and binding placement balanced to promote ski recovery. Lawson et al, did an interesting comparative study on snow in 1992. They measured post skate (SK) technique anterior compartment pressures with subjects using SK specific skis and then classic (CL) skis. The premise was that the extra swing weight of the CL skis while skating would elevate compartment pressures.

The results did indicate higher pressures using the CL skis to skate but were not statically significant. Unfortunately, the duration of each ski was only 10-12 minutes so these results do not translate well to most training plans. Intuitively, swing weight and the resultant load on our dorsiflexors to recover our ski back to midline many, many times during a ski could result in overdevelopment, strain, inflammation, excessive hypertrophy of the Anterior Tibialis, and resultant compartment volume compromise.
The ratchet mechanism on classic rollers adds significant weight to the front of the ski. Sprinting drills on CL rollers up hills should happen infrequently (think Kalebo). Volume double pole work on rollers can occur without ECS concerns. Using “combi” roller skis to SK with should be avoided or minimized, particularly in young athletes.
Boots should fit supportively and be technique specific. Overuse irritations due to medial/lateral stabilizing deficits while in skating in CL gear, or flexing a stiff SK boot during classic skiing are a concern.
Compression garments are contraindicated if excessively restrictive. They likely have limited ability to affect intramuscular metabolites during or after high intensity exercise (Rimaud D et al , Euro J Applied Physio). Temperature specific lower extremity clothing however, is always recommended to avoid vasoconstriction.
Technique cues while skiing, as well as video analysis, should focus on skiing relaxed and efficiently. While skating, make sure the athlete releases the foot/ankle at the conclusion of the lateral push phase. Tempo skiing up inclines helps decrease unwanted static foot/ankle postures in either discipline.
Core and hip strength must be addressed to avoid medial hip and knee “collapse”, resulting in ankle /foot torsions, thereby stressing the anterior musculature. Orthotics should be utilized for skiing and running in those athletes that pronate excessively (drop the mid foot) or have great toe (First Ray) mobility issues which are compensated for via lateral compartment activity (Peroneal Longus). Calf tightness is compensated for via pronation and our Anterior Tibialis (Dorsiflexor) will “fight” to suspend our mid foot if unchecked, yet another source of potential overuse. Please refer to a prior Nordic Solution piece on “reasons to stretch your calves”.

Any focused strengthening of compartments to improve resiliency in asymptomatic individuals should follow a high load, low rep and set format, as athletes get plenty of “reps” with functional training.

Massage, foam rolling and myofascial release work (with or without tools) have been shown to only delay symptoms in diagnosed individuals, but in unaffected athletes, likely does no harm and may have mechanically induced circulatory benefits. Electrical stimulation modalities provide a similar response.
Proper cool down is important to help assist with “clearing” undesirable metabolites. The literature seems to indicate a wide window of recovery parameters best suited to clear metabolites from tissue. Twenty minutes or less, at 30%-50% of VO2 max or 10%-50% of ventilatory threshold has been shown to best rid post exertion lactate (Riberio et al, Coso et al, Baldari et al ). Active recovery is more effective than massage, cryotherapy or any other modality for this task.
Icing the lower legs after strenuous workouts may provide minimal physiologic benefit but likely “does no harm” and provides parasympathetic based relief. Contrast baths have been shown to be more effective regarding metabolite clearing. A 3 (hot) to 1 (cold) time ratio is typically utilized (Viitasaio et al 2007, Versey et al 2010).

Cryocompressive garments, if available, are a useful adjunct to recovery (Jakeman et al, Euro J Appli Phys 2007) and in one animal study actually promoted neurovascular growth ( Dahl et al, J Ortho Res 2007).
Massage, foam rolling and myofascial release work (with or without tools) have been shown to only delay symptoms in diagnosed individuals, but in unaffected athletes, likely does no harm and may have mechanically induced circulatory benefits. Electrical stimulation modalities provide a similar response.
Potential sources of over work/use are easily addressed by the athlete and their coach without sacrificing training benefits provided imagination and logic prevail as summer training plans are designed. Have a productive summer!
